Makindo Medical Notes.com |
|
|---|---|
| Download all this content in the Apps now Android App and Apple iPhone/Pad App | |
| MEDICAL DISCLAIMER:The contents are under continuing development and improvements and despite all efforts may contain errors of omission or fact. This is not to be used for the assessment, diagnosis or management of patients. It should not be regarded as medical advice by healthcare workers or laypeople. It is for educational purposes only. Please adhere to your local protocols. Use the BNF for drug information. If you are unwell please seek urgent healthcare advice. If you do not accept this then please do not use the website. Makindo Ltd | |
Right Ventricular Outflow Tract Tachycardia (RVOT)
-
| About | Anaesthetics and Critical Care | Anatomy | Biochemistry | Cardiology | Clinical Cases | CompSci | Crib | Dermatology | Differentials | Drugs | ENT | Electrocardiogram | Embryology | Emergency Medicine | Endocrinology | Ethics | Foundation Doctors | Gastroenterology | General Information | General Practice | Genetics | Geriatric Medicine | Guidelines | Haematology | Hepatology | Immunology | Infectious Diseases | Infographic | Investigations | Lists | Microbiology | Miscellaneous | Nephrology | Neuroanatomy | Neurology | Nutrition | OSCE | Obstetrics Gynaecology | Oncology | Ophthalmology | Oral Medicine and Dentistry | Paediatrics | Palliative | Pathology | Pharmacology | Physiology | Procedures | Psychiatry | Radiology | Respiratory | Resuscitation | Rheumatology | Statistics and Research | Stroke | Surgery | Toxicology | Trauma and Orthopaedics | Twitter | Urology
Related Subjects: |Classical Ventricular Tachycardia |Idiopathic Ventricular Tachycardia |Right Ventricular Outflow Tract Tachycardia |Idiopathic Fascicular Left Ventricular Tachycardia |Left Ventricular Outflow Tract Tachycardia |Ventricular Fibrillation |Resuscitation - Adult Tachycardia Algorithm |Resuscitation - Advanced Life Support |Automatic Implantable Cardioverter Defibrillator (AICD)
Idiopathic ventricular tachycardia in patients with an anatomically normal heart is a distinct entity whose management and prognosis differs from ventricular tachycardia associated with structural heart disease.
About
- A form of Idiopathic ventricular tachycardia (IVT)
- 80% of Idiopathic ventricular tachycardia (IVT)
- Arises from the RV ventricle so LBBB
Aetiology
- Absence of structural heart disease
- Re-entrant arrhythmia
- Non sustained, repetitive, monomorphic VT
Criteria
- No structural heart disease
- No metabolic/electrolyte abnormalities
- No long QT syndrome can be found
RVOT
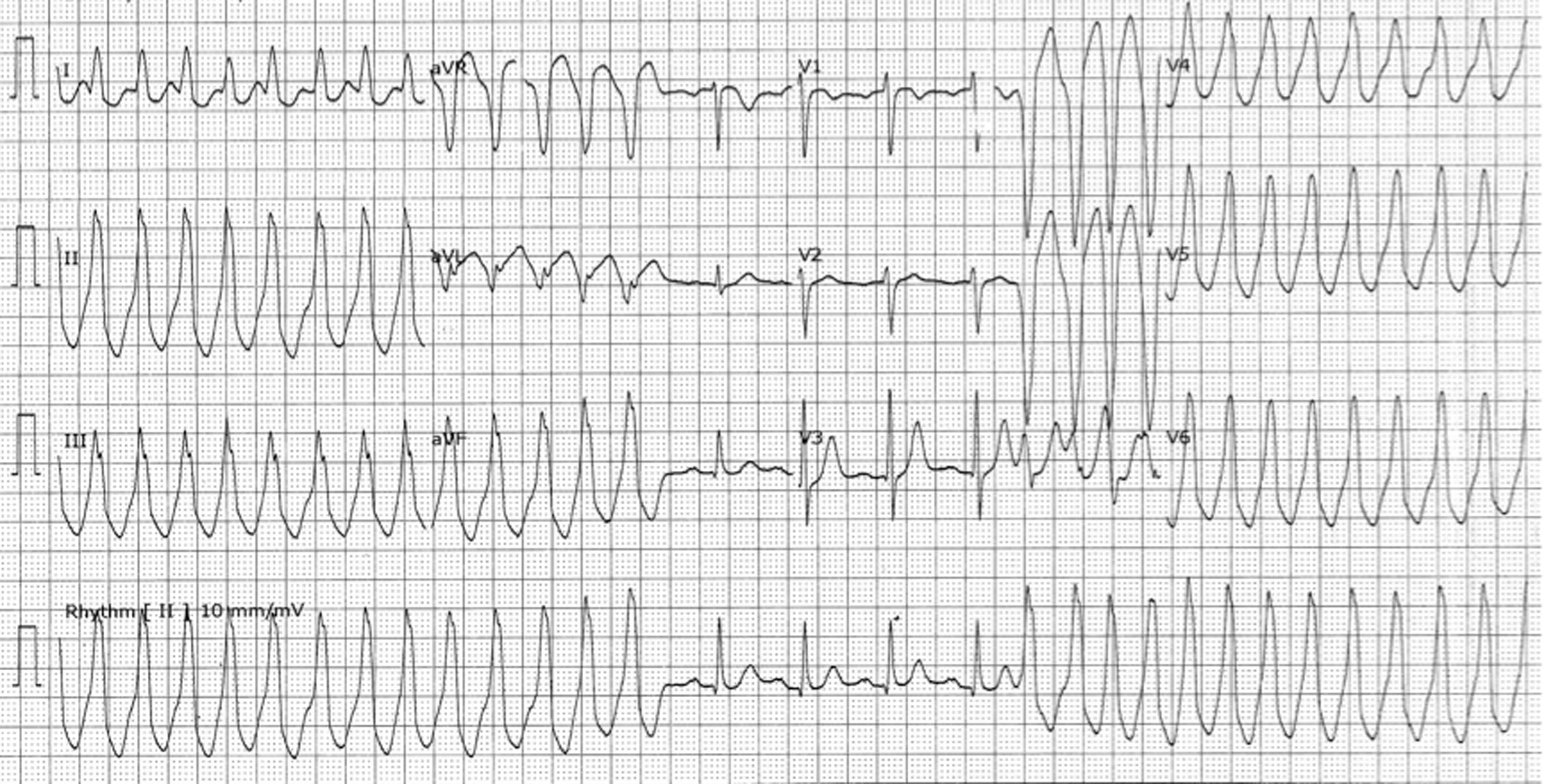
Clinical
- Commoner in females. Most commonly ages 30-50
- Paroxysmal, exercise-induced sustained VT.
- Syncope, palpitations
Investigations
- Bloods: normal, Echo: normal, CXR: normal
- ECG: RVOT VT has LBBB morphology and Axis is inferior with small r waves in V1. rS in V1 and R in V6. Note in ARVD the resting 12-lead ECG typically shows inverted T waves in right precordial leads and, when present, RV conduction delay with an epsilon wave, best seen in leads V1-V2.
- Exercise stress testing may provoke the arrhythmia
- MRI: MRI may show abnormalities of the RV in up to 70% of patients, including focal thinning, diminished systolic wall thickening and abnormal wall motion
Classical VT is by far the most common cause of wide complex regular tachycardia, and there is no perfectly reliable way to distinguish classic VT with all its dangers from idiopathic VT or SVT with aberrancy on the surface 12-lead ECG.
Management: Treat as Classical VT with Adult Tachycardia arrhythmia
- ABC. If unsure and Idiopathic VT diagnosis not known then follow Adult Tachycardia pathway. An early echo is very useful to assess LV function.
- It can be terminated with Adenosine 6-24 mg as advised by senior cardiologist (ineffective if patient has Arrhythmogenic Right Ventricular Dysplasia as the underlying cause).
- Before using verapamil get echo first to show normal LV. If compromised then DC shock.
- Under specialist senior cardiology supervision IV Verapamil 10 mg over 3-5 mins. Ensure normal Echo first and good LV function and contractility. Be read to DC convert if needed. If compromised then DC shock.
- Beta blockers may be used. Long term RF Ablation can be used