Related Subjects:
|Pasteurella Multocida
|Capnocytophaga canimorsus
|Snake Bites
|Dog Bites
|Tetanus
When the spores are exposed to a
favorable environment, such as water and sugar, the bacterium can
become active again.
| Initial Tetanus Management Summary |
|---|
|
ABC, Manage airway if Laryngeal spasm. May need ITU
Sedation , neuromuscular blockade, IV Benzodiazepine
Tetanus Immune globulin before would debridement
Give IV Metronidazole. Vaccinate.
|
About
- A bacterium that can generally be found in the
soil everywhere
- A cause of death due to the toxin release Tetanospasmin with spastic paralysis
- It is more a problem in developed countries with a lack of immunisation and poor wound care.
- Tetanus is one of the few bacterial diseases that does not confer immunity following recovery from acute illness, all patients with tetanus require active immunization
Fatality is 20 to 60%
Microscopy
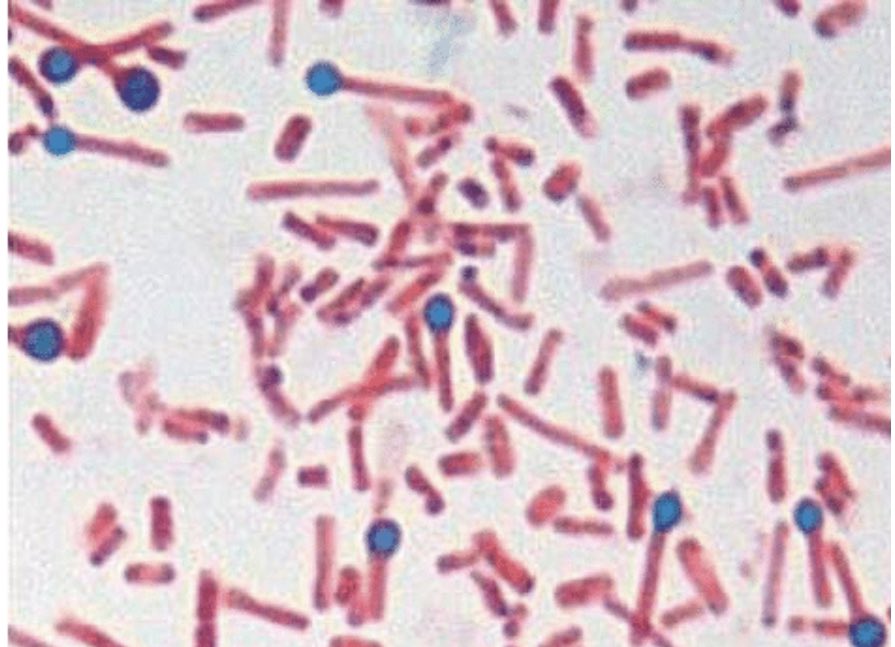
Characteristics
- Gram positive motile obligate anaerobic found in soil
- Terminal spore-forming drumstick appearance bacillus
- Produces 2 neurotoxins - tetanospasmin and tetanolysin.
Aetiology
- Spores are found in human and animal faeces and in the soil and can enter open wounds and flourish in deep wounds with low oxygenation with spore germination and toxin formation
- Only 0.01 g of metalloproteinase Tetanospasmin "tetanus toxin" can be lethal.
- It is a zinc-dependent matrix metalloproteinases that enters the pre synapse of the lower motor neuron using retrograde axonal transport that passes up to the spinal cord and brain stem where it blocks GABA and glycine mediated inhibition leading to spasms.
- It takes approximately 2 weeks to travel up the axon so ask about an injury 2 weeks ago and the usual duration of clinical tetanus is four to six weeks
Clinical
- Recent wound which may have some necrosis which is contaminated and deep
- Headache, malaise, fever
- Muscles
- Muscles become stiff and contract
- Trismus (lockjaw) and spasm of facial muscles.
- Risus sardonicus (sardonic smile)
- Generalised muscle spasms
- Back Erector spinae muscles contract opisthotonus
- Respiratory muscles contract
- Laryngeal muscles - can occlude airway
- Autonomic
- Tachycardia, High BP
- High temperature
- Sweating, salivation
- Infection from puncture wounds, lacerations, surgery, burns, bites,
- Neonates as a tradition to rub soil on the umbilical stump of the newborn.
- Incubation period can be from a few days to months
- Generalized, local, Cephalic, Neonatal
- Risus sardonicus, lock jaw (Trismus), opisthotonus
Grading of Tetanus
- I (mild)-trismus and generalized
stiffness without respiratory
embarrassment or spasms
- II (moderate)-marked rigidity, brief
spasms, mild respiratory embarrassment,
and dysphagia
- III and IV-frequent prolonged spasms,
respiratory embarrassment with apnoeic
spells, severe dysphagia. and
cardiovascular abnormalities
Differential
- Strychnine poisoning, in which glycine is antagonized so levels should be sent if suspected.
- Acute dystonia may present with trismus and so benztropine may be given to excluding this.
Investigations
- Fine film of growth on blood agar without discrete colonies
- Detection of circulating toxin
Sensitivity
Prevention
- Those who have not had Clostridium tetani immunisation should receive tetanus Ig. This gives passive immunisation of any person with a wound that may be contaminated with tetanus spores
- Prophylaxis: 250 Units IM (single dose) or Active tetanus: 3000-6000 Units IM
- Clean minor wound: # doses unknown or 0-2 doses; toxoid only. >3 doses; toxoid if >10 years ago
- All other wounds. # doses unknown or 0-1 doses; toxoid plus IG. 2 doses; toxoid, but no IG if wound <24 hours old. >3 doses; toxoid if >5 years ago, and no IG
Tetanus toxoid vaccination for active cover
- Used for tetanus immunisation. A booster injection in a previously immunised patient can help prevent this potentially lethal syndrome.
- Used to induce active immunity against tetanus in selected patients. Need to administer booster doses to maintain immunity throughout life.
Management
- ABC, may need tracheotomy. Neuromuscular blockade. It is not spread by person to person so isolation not warranted
- General Sedation and muscle relaxation and oral or IV diazepam can be given. Seizures may occur see Status epilepticus. VTE prophylaxis.
- In severe cases ventilatory support and IV sedation and ITU support are required.
- Give either to bind toxin and tetanus toxoid vaccine before manipulating the wound.
- Human tetanus immunoglobulin 150 U/kg IM over multiple sites
- Equine Tetanus Immune globulin 500-1000 u/kg IM
- Both carry risk of anaphylaxis
- Immediate treatment is to scrub the wound clear of any residual toxin and infection and debridement after Tetanus Immune globulin has been given.
- Give antibiotics for the wound Metronidazole 500 mg IV TDS
Complications
- Autonomic instability - As well as the severe spasms there is also neural induced overstimulation of the sympathetic system which is usually nowadays managed with good ITU support for respiratory issues is now the commonest cause of death.
- Hypotension and hypertension are seen as well as other manifestations of autonomic dysfunction. Sympathetic overdrive managed with IV labetalol. Inotropes may be needed for hypotension.
