Makindo Medical Notes.com |
|
|---|---|
| Download all this content in the Apps now Android App and Apple iPhone/Pad App | |
| MEDICAL DISCLAIMER:The contents are under continuing development and improvements and despite all efforts may contain errors of omission or fact. This is not to be used for the assessment, diagnosis or management of patients. It should not be regarded as medical advice by healthcare workers or laypeople. It is for educational purposes only. Please adhere to your local protocols. Use the BNF for drug information. If you are unwell please seek urgent healthcare advice. If you do not accept this then please do not use the website. Makindo Ltd | |
ECG - ST Elevation Myocardial Infarction STEMI
-
| About | Anaesthetics and Critical Care | Anatomy | Biochemistry | Cardiology | Clinical Cases | CompSci | Crib | Dermatology | Differentials | Drugs | ENT | Electrocardiogram | Embryology | Emergency Medicine | Endocrinology | Ethics | Foundation Doctors | Gastroenterology | General Information | General Practice | Genetics | Geriatric Medicine | Guidelines | Haematology | Hepatology | Immunology | Infectious Diseases | Infographic | Investigations | Lists | Microbiology | Miscellaneous | Nephrology | Neuroanatomy | Neurology | Nutrition | OSCE | Obstetrics Gynaecology | Oncology | Ophthalmology | Oral Medicine and Dentistry | Paediatrics | Palliative | Pathology | Pharmacology | Physiology | Procedures | Psychiatry | Radiology | Respiratory | Resuscitation | Rheumatology | Statistics and Research | Stroke | Surgery | Toxicology | Trauma and Orthopaedics | Twitter | Urology
Related Subjects: |ECG Basics |ECG Axis |ECG Analysis |ECG LAD |ECG RAD |ECG Low voltage |ECG Pathological Q waves |ECG ST/T wave changes |ECG LBBB |ECG RBBB |ECG short PR |ECG Heart Block |ECG Asystole and P wave asystole |ECG QRS complex |ECG ST segment |ECG: QT interval |ECG: LVH |ECG RVH |ECG: Bundle branch blocks |ECG Dominant R wave in V1 |ECG Acute Coronary Syndrome |ECG Narrow complex tachycardia |ECG Ventricular fibrillation |ECG Regular Broad complex tachycardia |ECG Crib sheets
Differentials
Acute Anterolateral MI
Acute anterolateral MI is recognised by ST-segment elevation in leads I, aVL and the precordial leads overlying the anterior and lateral surfaces of the heart (V3 - V6). Generally speaking, the more significant the ST elevation, the more severe the infarction. There is also a loss of general R wave progression across the precordial leads and there may be symmetric T wave inversion as well. Anterolateral myocardial infarctions frequently are caused by occlusion of the proximal left anterior descending coronary artery, or combined occlusions of the LAD together with the right coronary artery or left circumflex artery. Arrhythmias which commonly preclude the diagnosis of anterolateral MI on ECG and therefore possibly identify high-risk patients include right and left bundle branch blocks, hemiblocks and type II second degree atrioventricular conduction blocks.
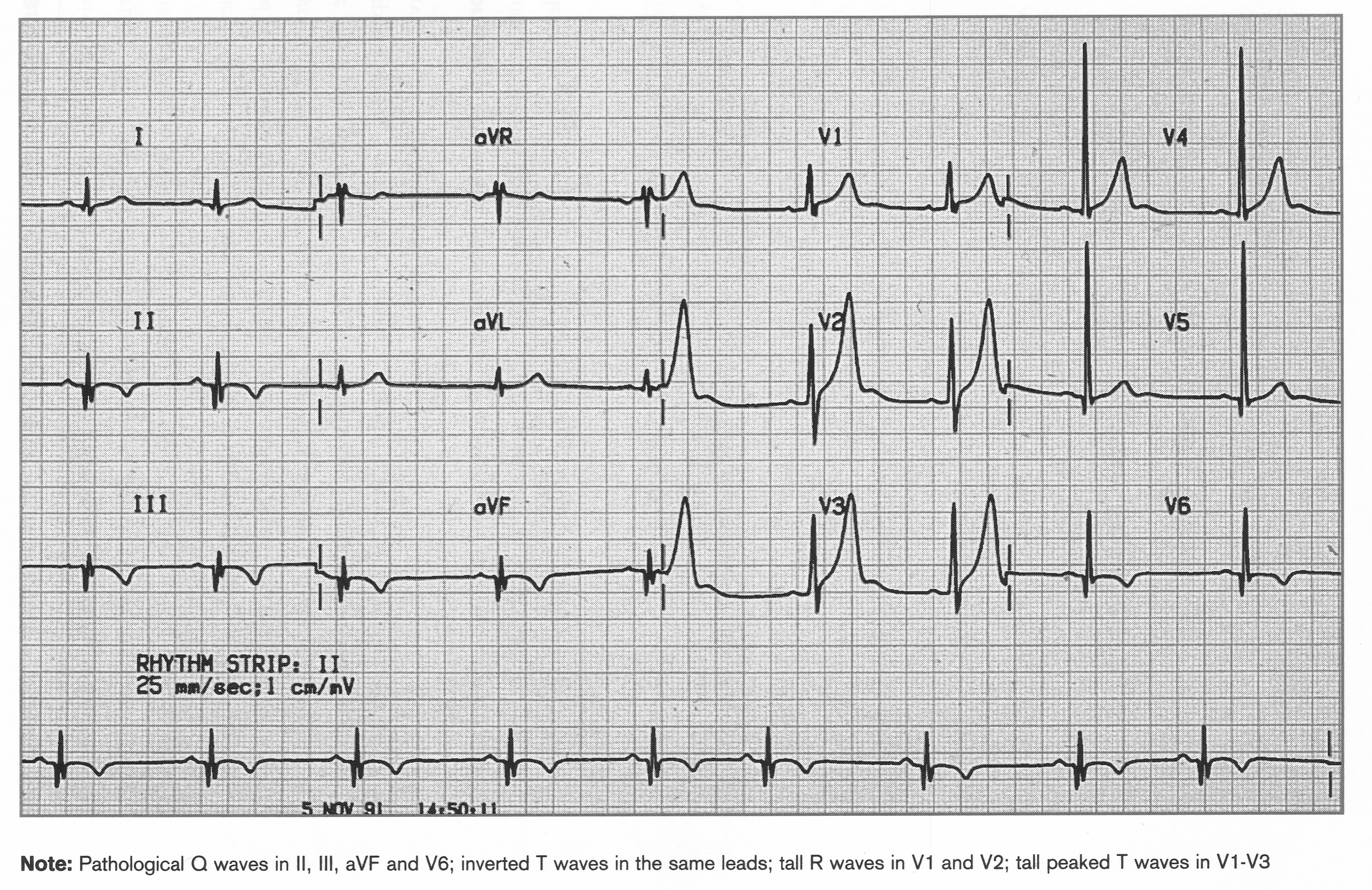
Acute inferior and posterior MI
Leads II, III and aVF reflect electrocardiogram changes associated with acute infarction of the inferior aspect of the heart. ST-elevation, developing Q waves and T wave inversion may all be present depending on the timing of the ECG relative to the onset of myocardial infarction. Most frequently, inferior MI results from occlusion of the right coronary artery. Conduction abnormalities that may alert the physician to patients at risk include second degree AV block and complete heart block together with junctional escape beats. Note that the patient below is also suffering from a concurrent posterior wall infarction as evidenced by ST depression in leads V1 and V2.
When examining the ECG from a patient with a suspected posterior MI, it is important to remember that because the endocardial surface of the posterior wall faces the precordial leads, changes resulting from the infarction will be reversed on the ECG. Therefore, ST segments in leads overlying the posterior region of the heart (V1 and V2) are initially horizontally depressed. As the infarction evolves, lead V1 demonstrates an R wave (which in fact represents a Q wave in reverse). Note that the patient below is also suffering from an inferior wall myocardial infarction as evidenced by ST elevation in leads II, III and aVF.
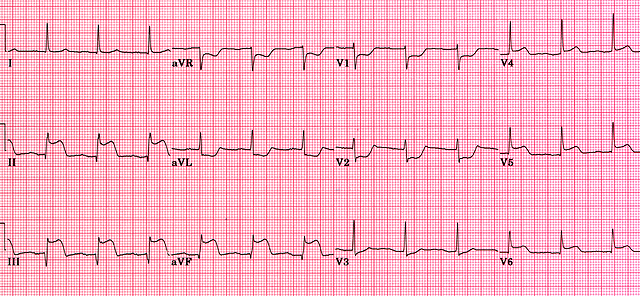
Acute right ventricular MI
In patients presenting with acute right ventricular MI, abnormalities in the standard 12 lead ECG are restricted to ST elevation greater than or equal to 1 mm in lead aVR. Although isolated right ventricular MI is usually seen in patients suffering from chronic lung disease together with right ventricular hypertrophy, it can occur in patients suffering a transmural infarction of the inferior-posterior wall which extends to involve the right ventricular wall as well. Right ventricular MI is most commonly caused by obstruction of the proximal right coronary artery and is frequently associated with right bundle branch block. Furthermore, only 5% - 10% of patients suffer from haemodynamic symptoms.
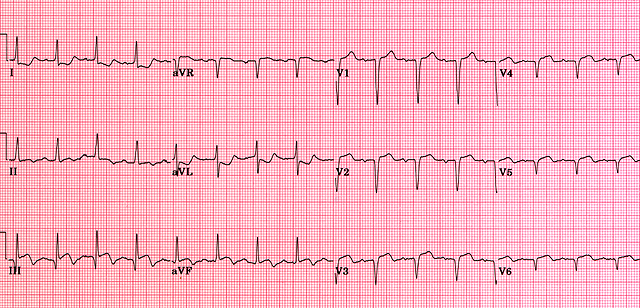
Acute septal MI
Acute septal MI is associated with ST elevation, Q wave formation and T wave inversion in the leads overlying the septal region of the heart (V2 and V3).
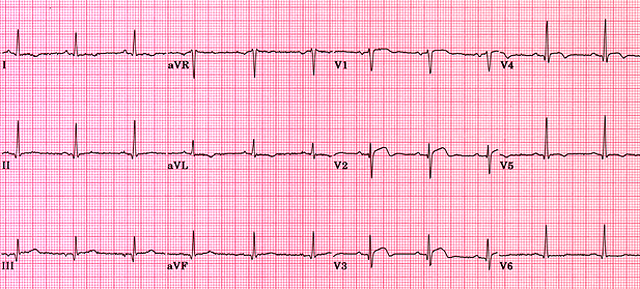
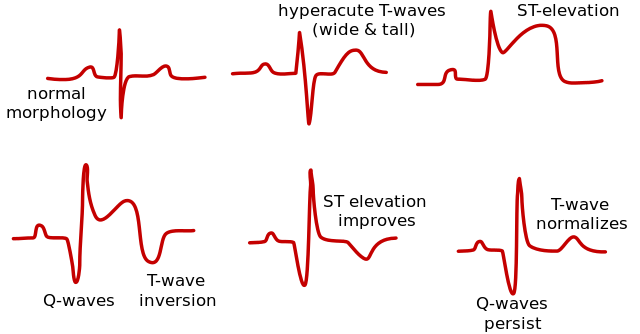
ST elevation in the setting of chest pain must be treated as a medical emergency and possible STEMI
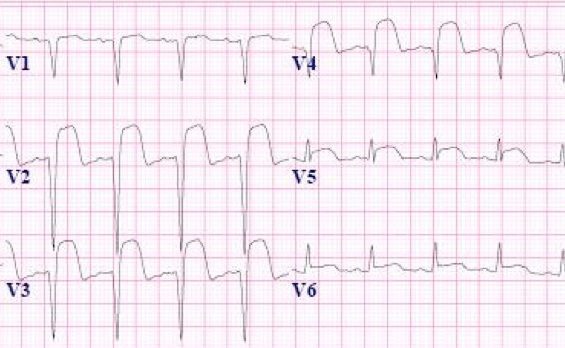 Anterior STEMI with tombestoning
Anterior STEMI with tombestoning
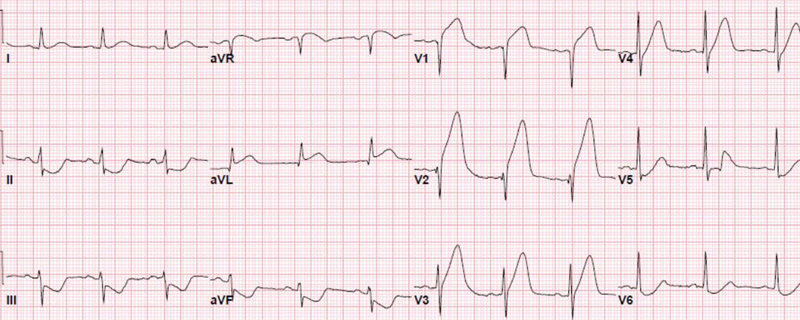 Anterior STEMI with tombestoning
Anterior STEMI with tombestoning
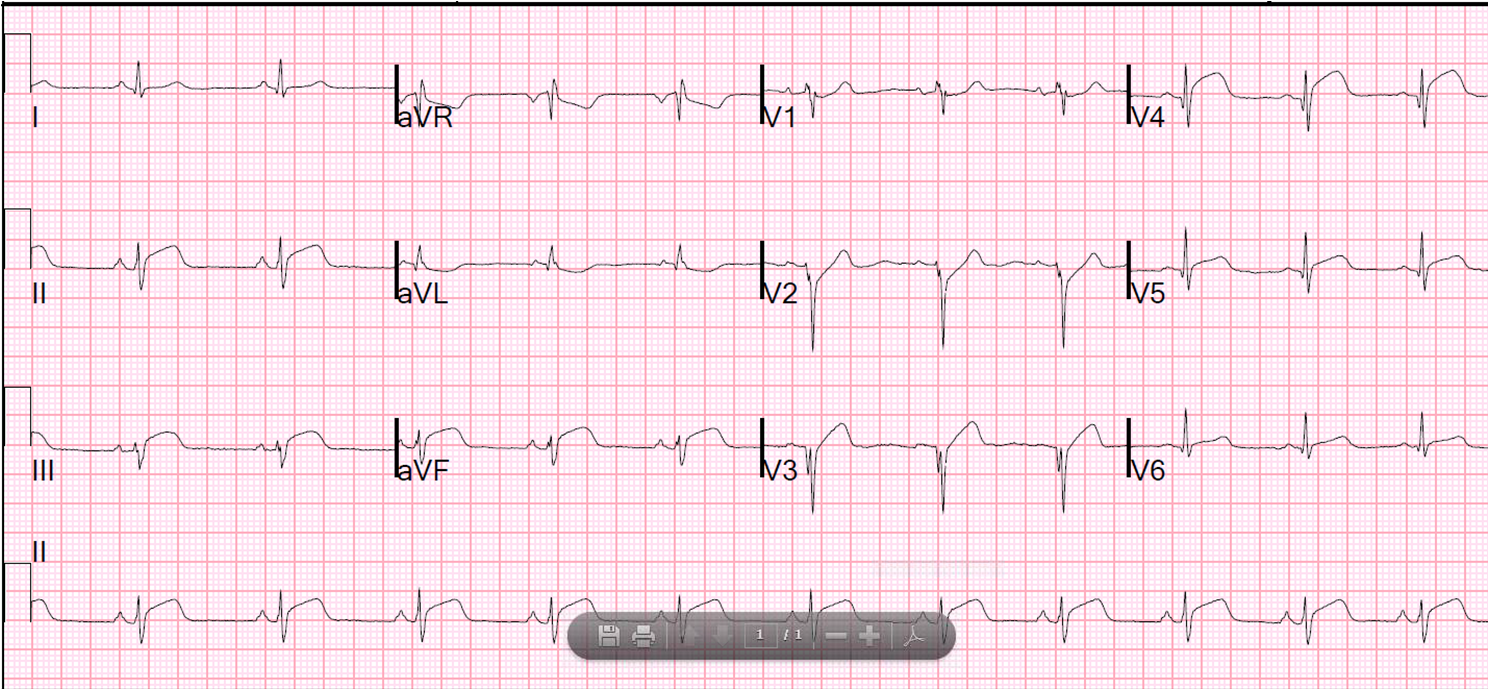
Others
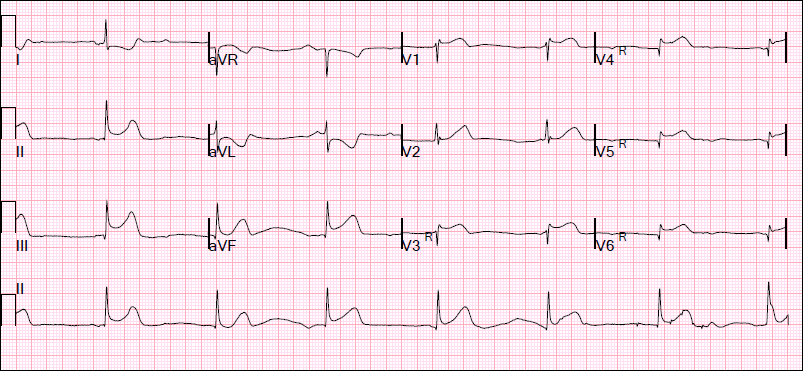
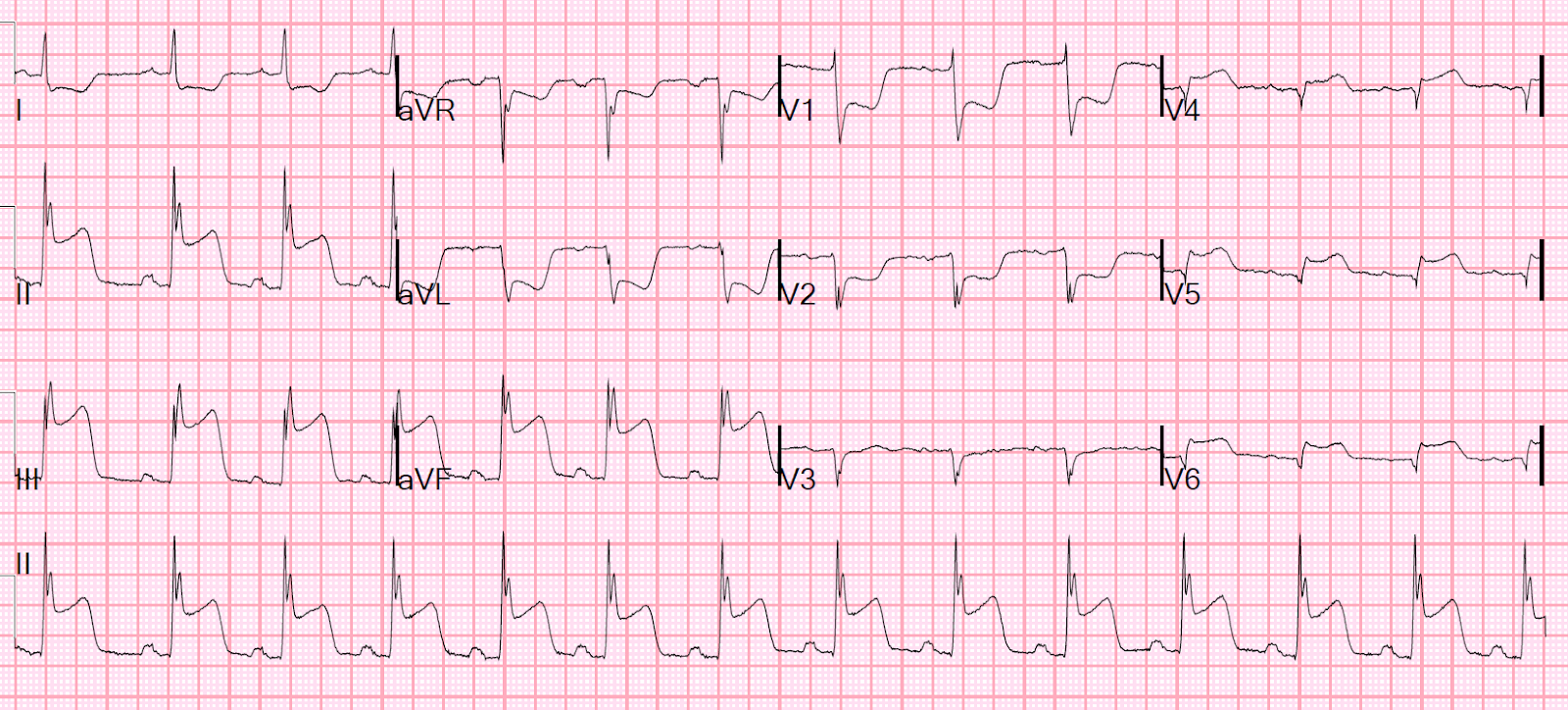
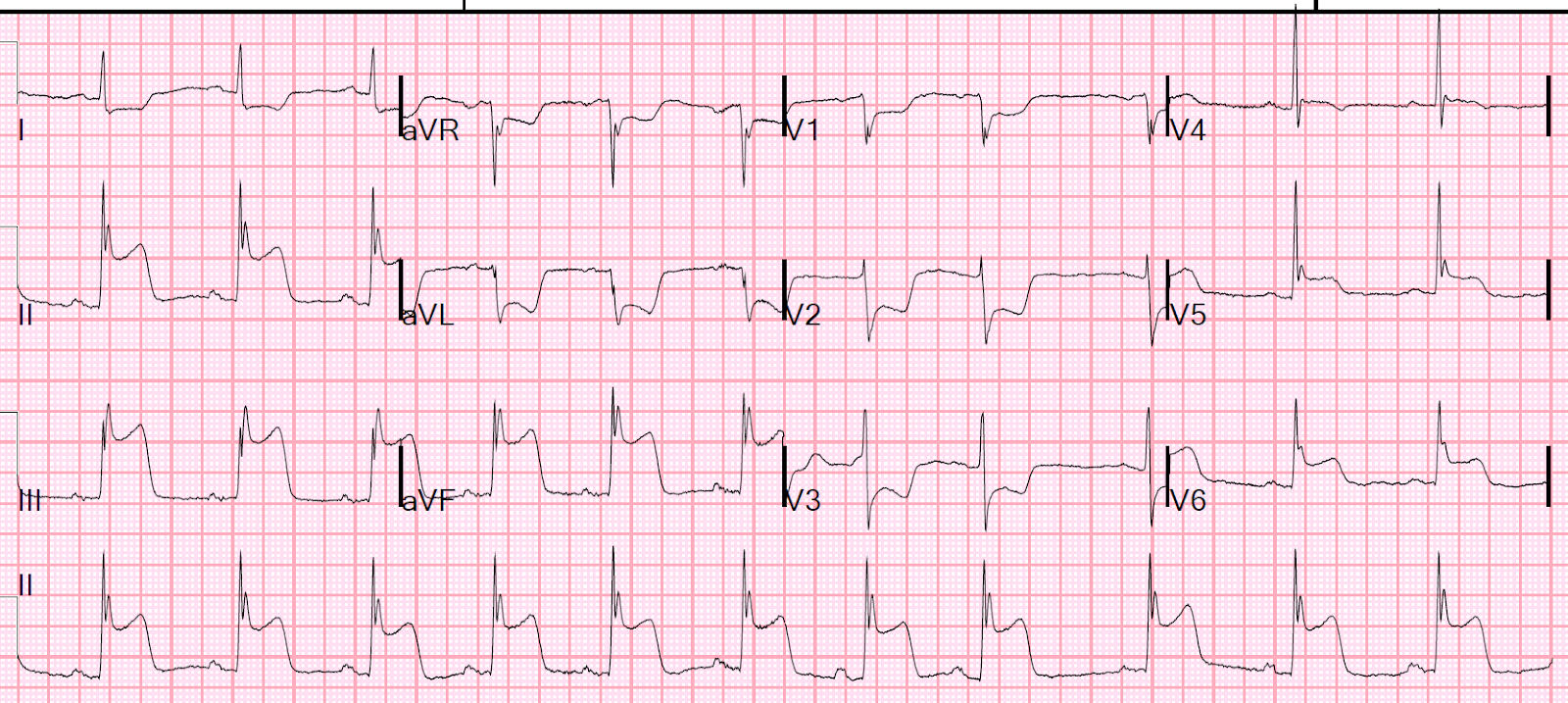
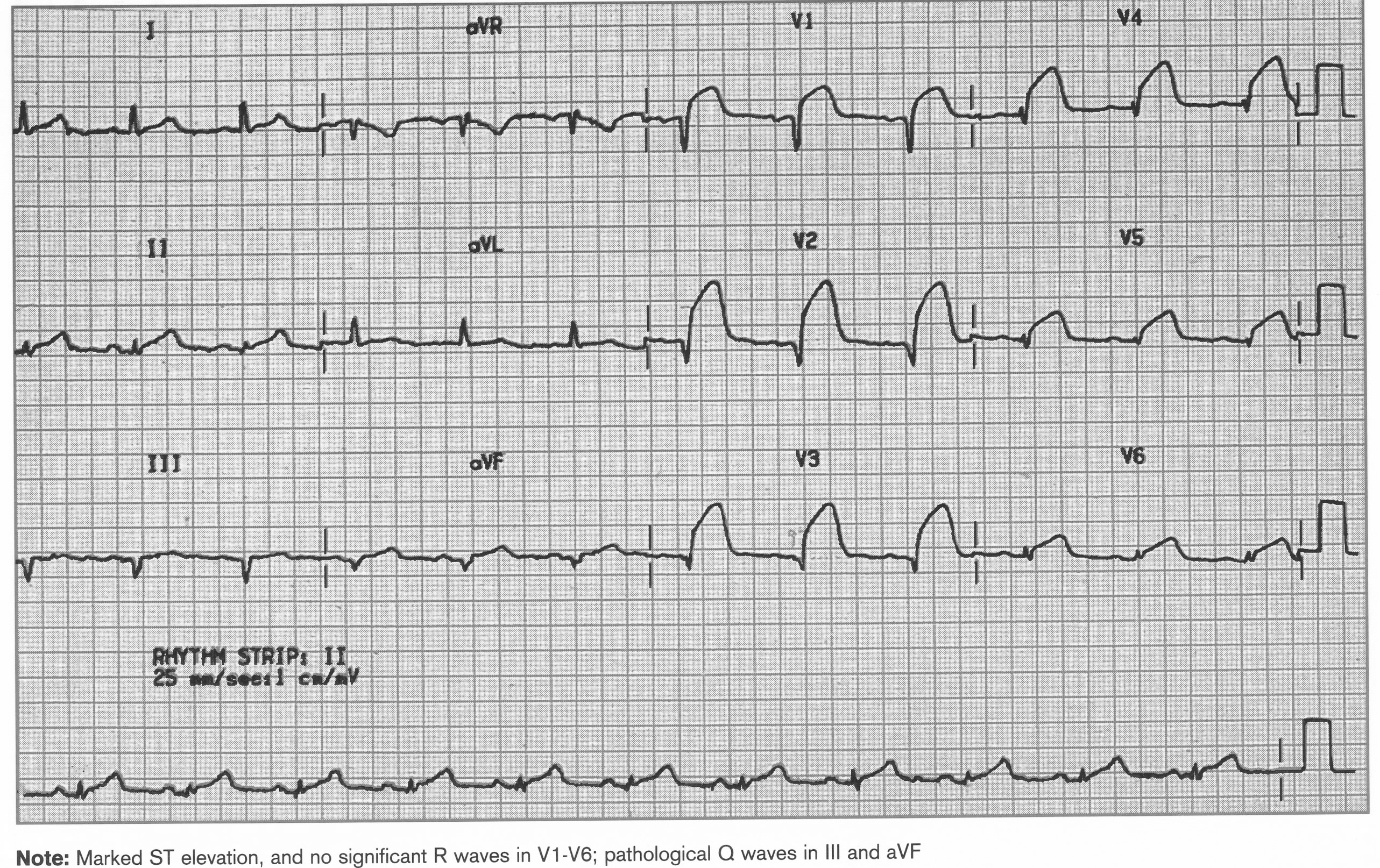
Acute Anterior STEMI, old inferior MI
ST elevation, no R waves V1-V6, Pathological Q waves in III and aVF
Recent Anterior-lateral STEMI
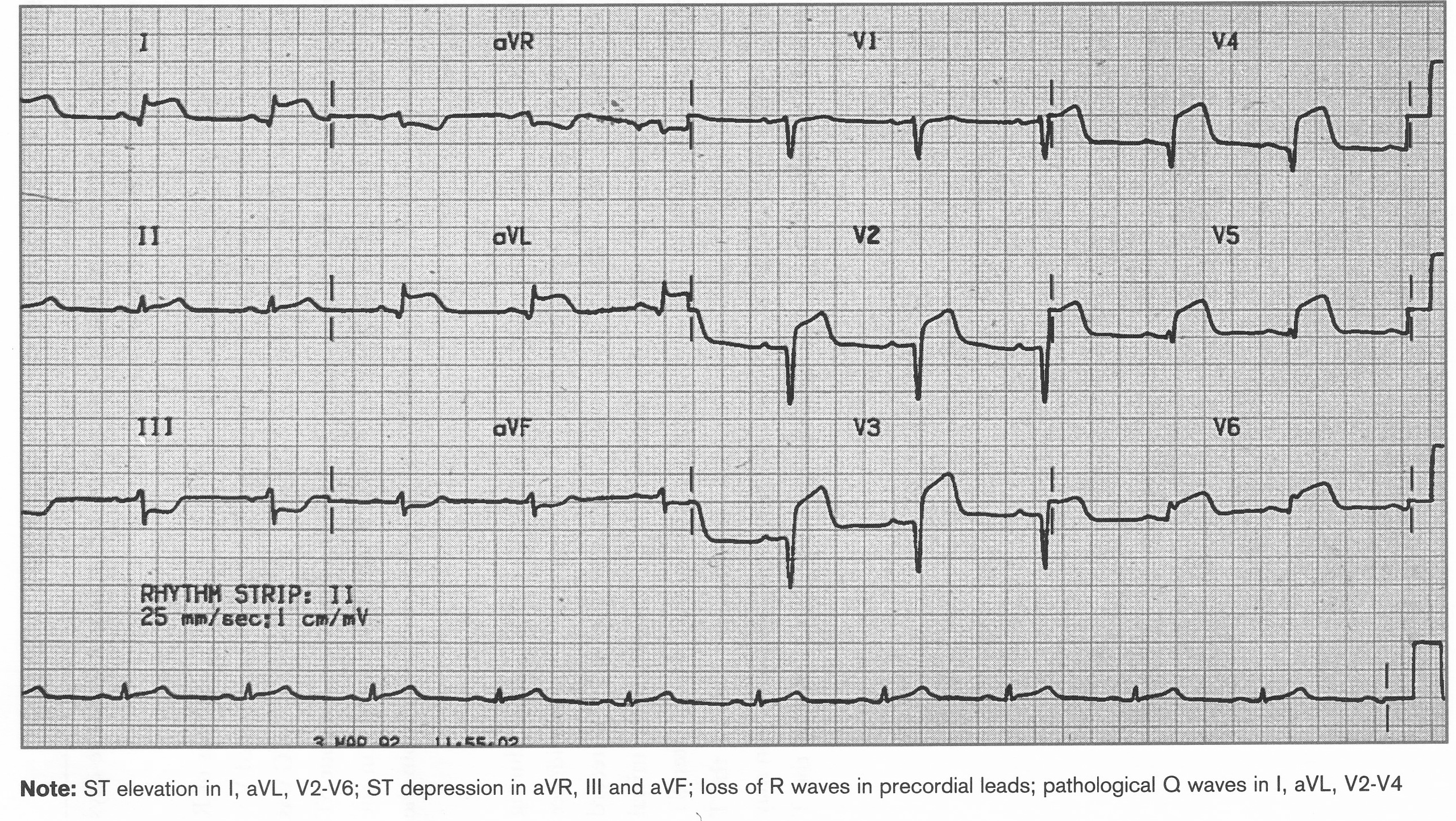
ST elevation I, aVL, V2-V6, ST depression a VR, III, aVF. Loss of R waves, path Q waves I,aVL, V2-V4
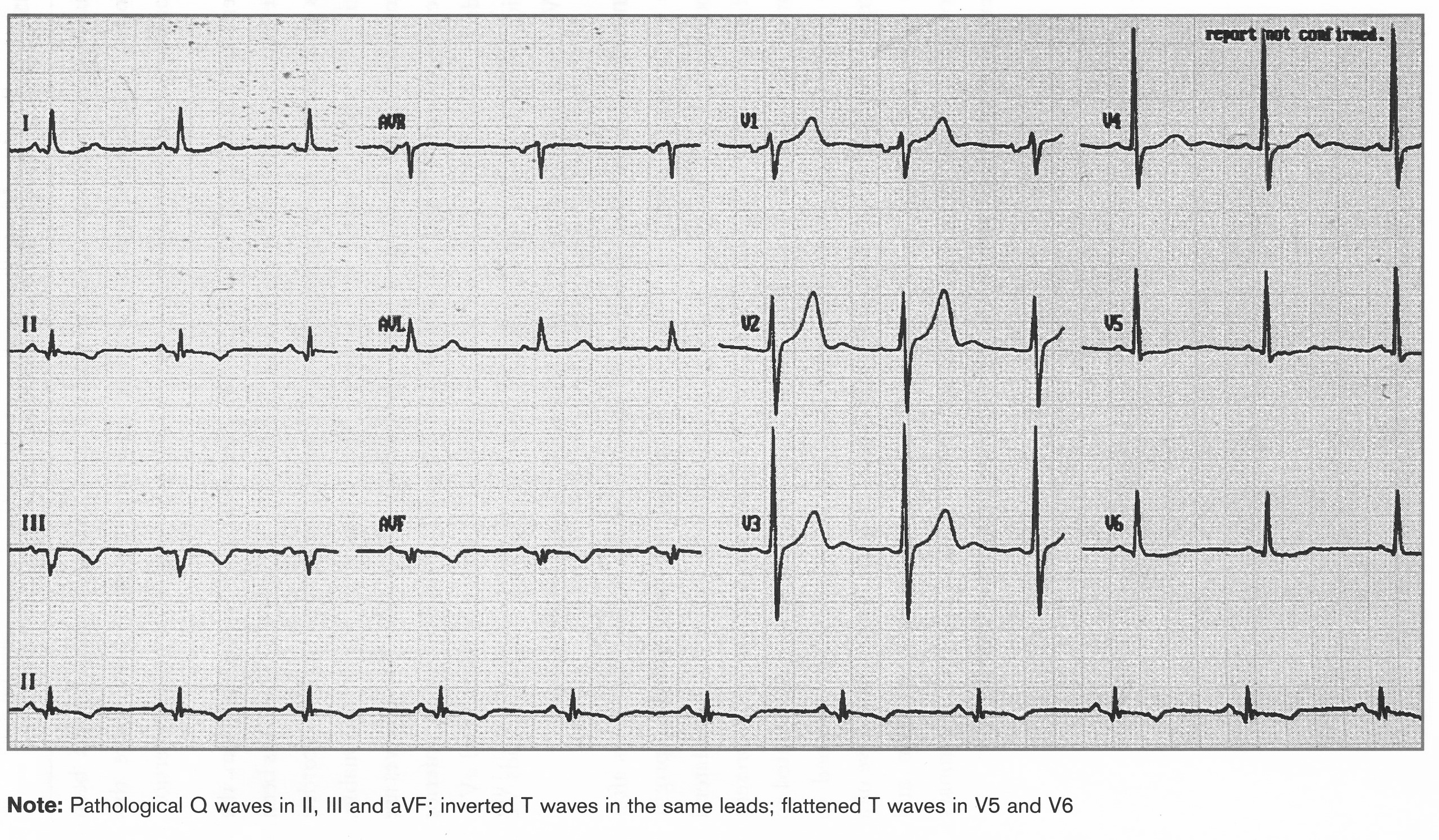
Old Inferior STEMIM
Pathological Q waves in II, III, aVF with inverted T waves. Flattened T waves in V5=V6
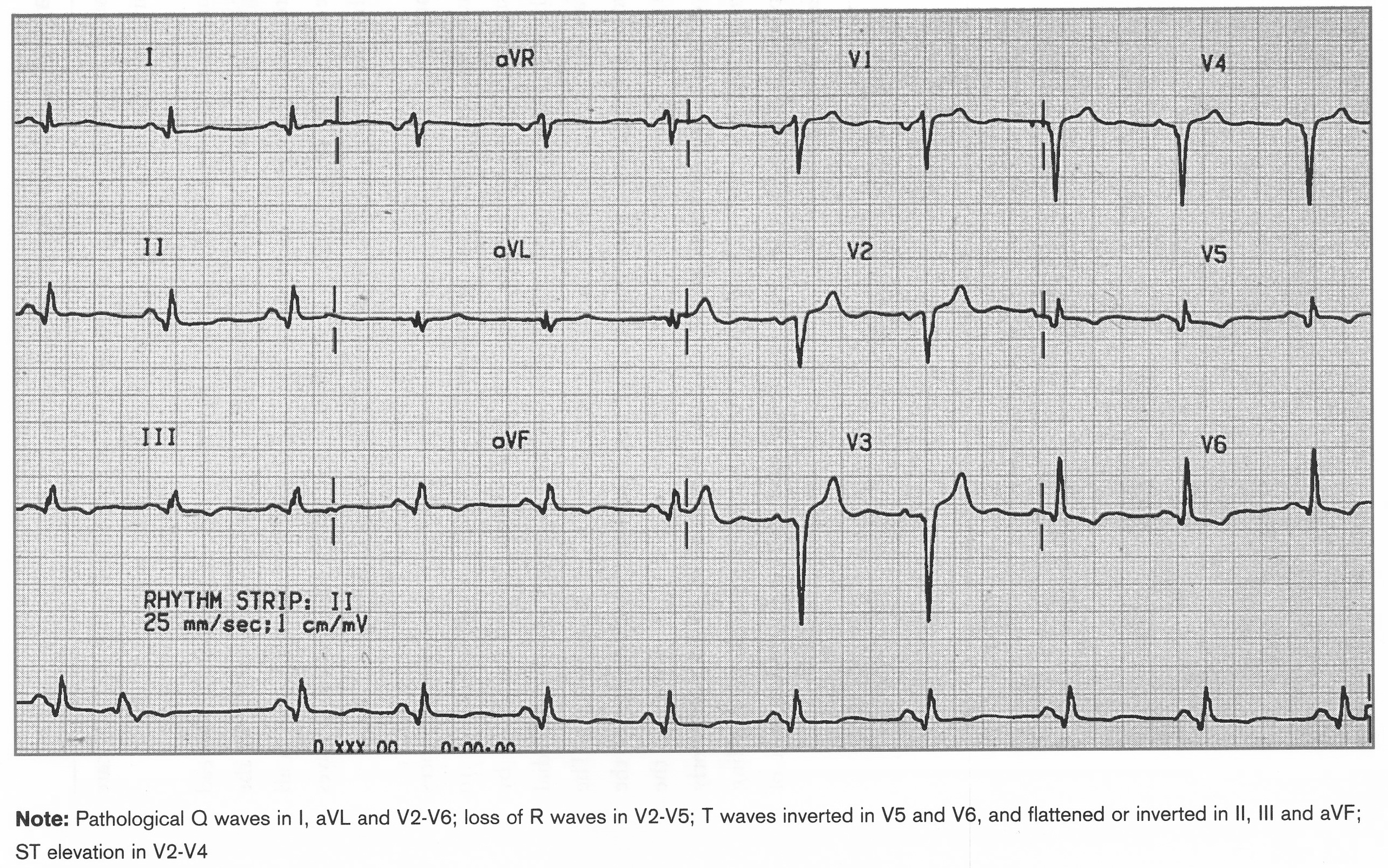
Old Anterolateral MI
Pathological Q waves in I,aVl, V2-6, Loss of R waves V2-5, T waves inverted V5-6 and flattened or inverted in II,III, avF, ST elevation V2-4
Acute Inferior STEMI
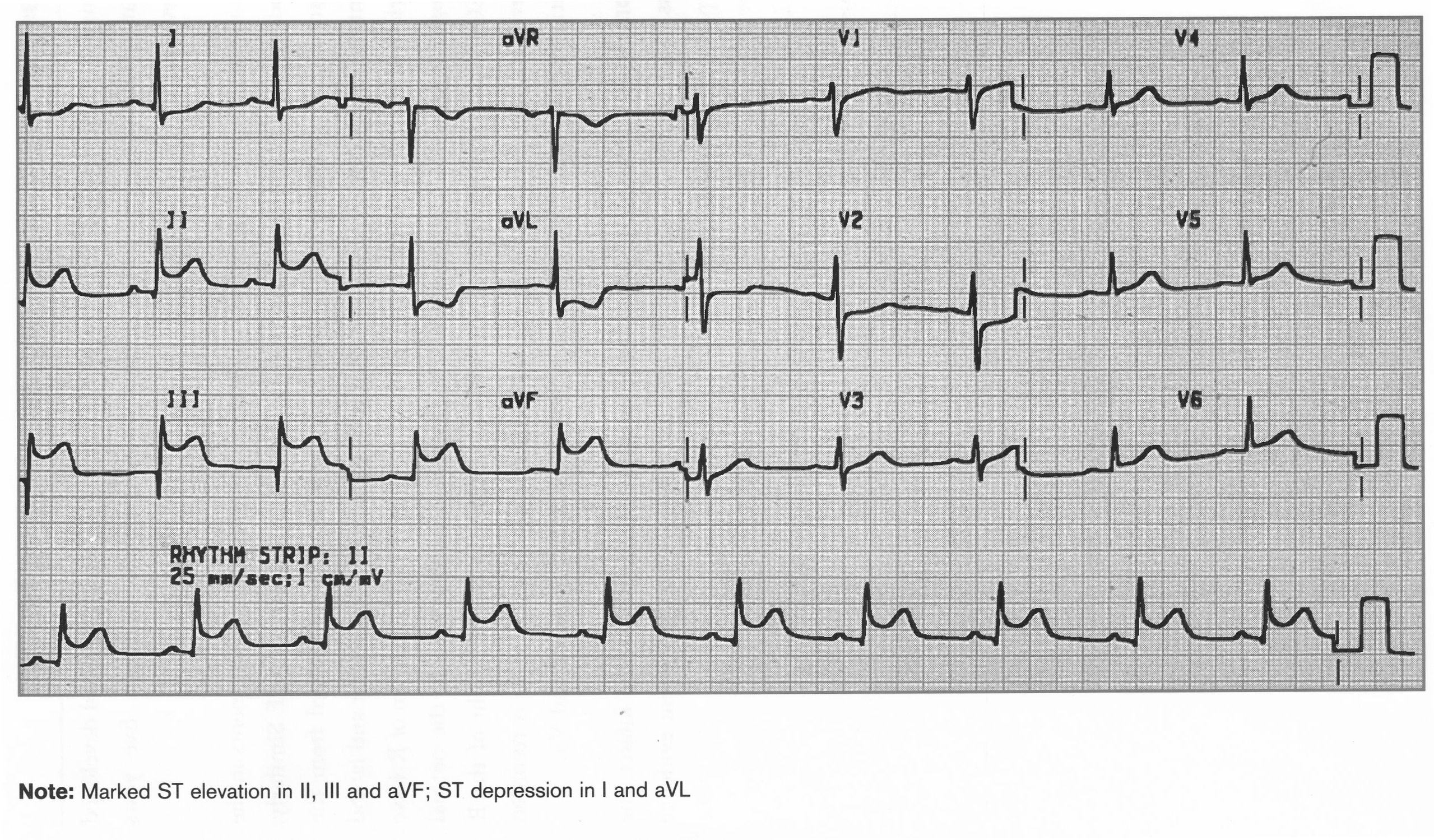
Acute Inferolateral MI
ST elevation I, II, aVF, aVL, V3-V6, Pathological Q wave in aVL
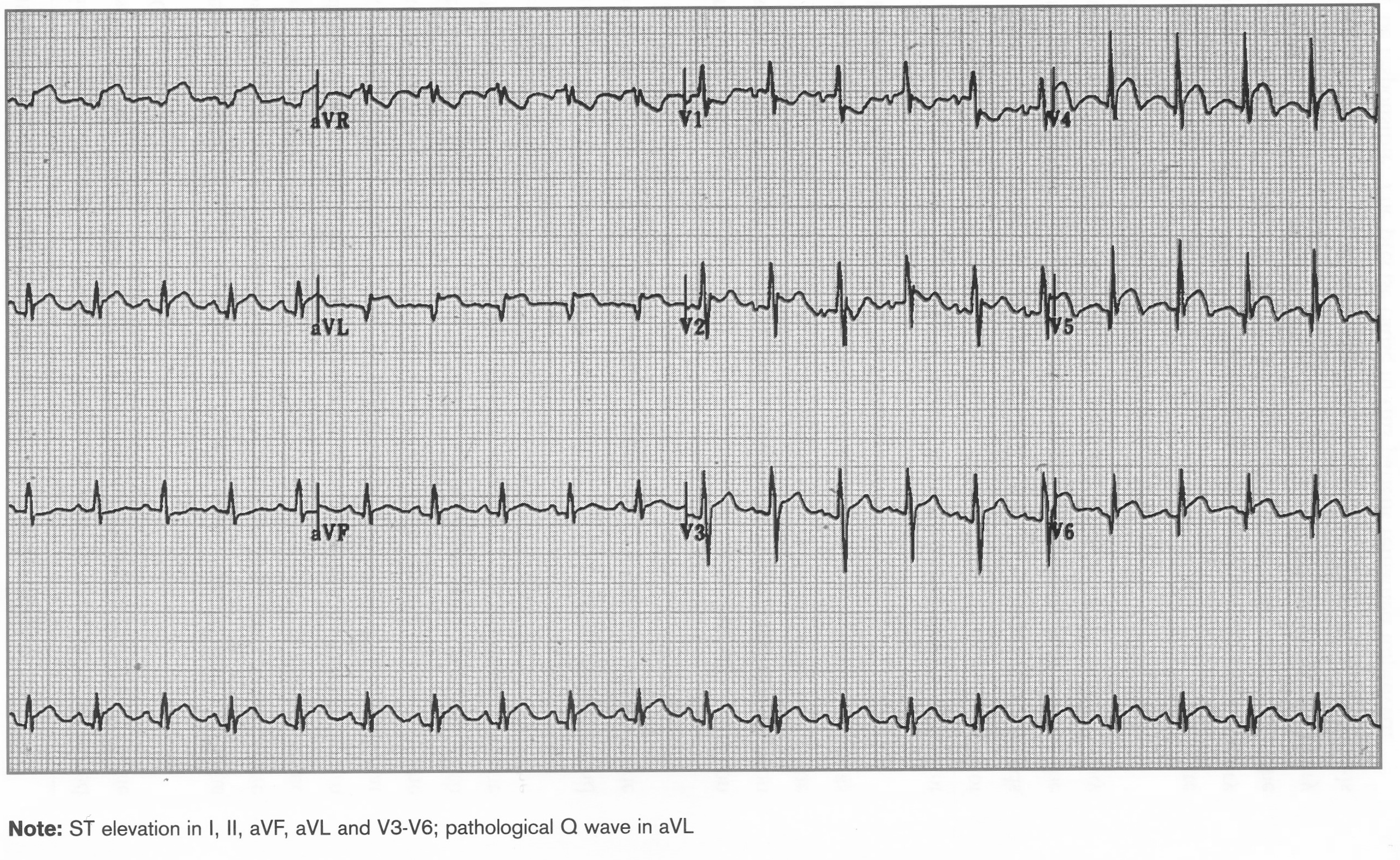
Acute Inf MI and True Posterior