Makindo Medical Notes.com |
|
|---|---|
| Download all this content in the Apps now Android App and Apple iPhone/Pad App | |
| MEDICAL DISCLAIMER:The contents are under continuing development and improvements and despite all efforts may contain errors of omission or fact. This is not to be used for the assessment, diagnosis or management of patients. It should not be regarded as medical advice by healthcare workers or laypeople. It is for educational purposes only. Please adhere to your local protocols. Use the BNF for drug information. If you are unwell please seek urgent healthcare advice. If you do not accept this then please do not use the website. Makindo Ltd | |
Pyoderma gangrenosum
-
| About | Anaesthetics and Critical Care | Anatomy | Biochemistry | Cardiology | Clinical Cases | CompSci | Crib | Dermatology | Differentials | Drugs | ENT | Electrocardiogram | Embryology | Emergency Medicine | Endocrinology | Ethics | Foundation Doctors | Gastroenterology | General Information | General Practice | Genetics | Geriatric Medicine | Guidelines | Haematology | Hepatology | Immunology | Infectious Diseases | Infographic | Investigations | Lists | Microbiology | Miscellaneous | Nephrology | Neuroanatomy | Neurology | Nutrition | OSCE | Obstetrics Gynaecology | Oncology | Ophthalmology | Oral Medicine and Dentistry | Paediatrics | Palliative | Pathology | Pharmacology | Physiology | Procedures | Psychiatry | Radiology | Respiratory | Resuscitation | Rheumatology | Statistics and Research | Stroke | Surgery | Toxicology | Trauma and Orthopaedics | Twitter | Urology
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
Every ulcerated skin lesion ask could this be Pyoderma Gangrenosum. PG is a rare, non-infectious, inflammatory skin condition characterized by painful ulcers. It is often associated with systemic diseases like inflammatory bowel disease (IBD), rheumatoid arthritis, and haematologic disorders,
About
- Can easily be dismissed as just another ulcer.
- Always consider other causes than the common venous leg ulcer.
- Always be on the lookout for skin cancers and other diseases masquerading as simple venous ulcers.
- If in doubt dermatology referral and biopsy.
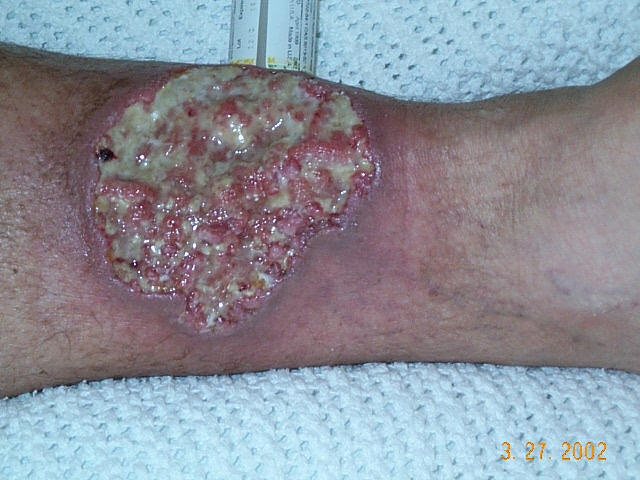 Image
Image
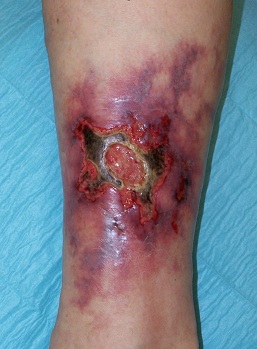
Clinical
- Pain: Very Painful ulcers compared to appearance and can progress rapidly
- Edge: Violaceous or bluish undermined borders.
- Base: Necrotic with a purulent, granulomatous appearance.
- Size: Lesions can vary in size from a few centimeters to large, rapidly expanding ulcers.
- Ulcer may even occur around a colostomy or recent surgery.
- Type of skin lesion preceding the ulcer (papule, pustule, or vesicle)
- Possibly minor trauma (pathergy) preceding development of the ulcer
- Coexisting disease - RA, Ulcerative colitis, Myeloma etc.
- Drugs: hydroxyurea, or granulocyte-macrophage colony-stimulating factor)
Causes
- Idiopathic in 20%
- Inflammatory bowel disease
- Lymphoma and Leukaemia, Multiple myeloma
- Primary biliary cirrhosis
- Rheumatoid arthritis
- Myeloproliferative disorders, leukaemia.
- Hepatitis, HIV, and monoclonal gammopathies.
Investigations
- FBC, WCC, ESR and CRP elevated.
- Skin biopsy: neutrophilic infiltrates in the dermis and epidermis, not pathognomonic. Exclude infection.
- No specific laboratory test confirms PG. Test for IBD, RA, Leukaemia
Management
- Avoid trauma. Skin grafts and surgery can make things worse with enlargement of the ulcer.
- Topical strong steroid preparations or calcineurin inhibitors (tacrolimus) applied to affected skin.
- Pain Management: Adequate pain control is critical, often requiring strong analgesics.
- Wound Care: non-adhesive dressings, to promote healing and prevent infection.
Systemic treatments
- Systemic corticosteroids are the first-line treatment for moderate to severe PG.
- Immunosuppressive Agents: Ciclosporin, Methotrexate as a steroid-sparing agent.
- Biologics: TNF-alpha inhibitors (e.g., infliximab, adalimumab) are effective, especially in refractory cases or when associated with IBD.
- Antibiotics: Not typically required unless there is a secondary bacterial infection.